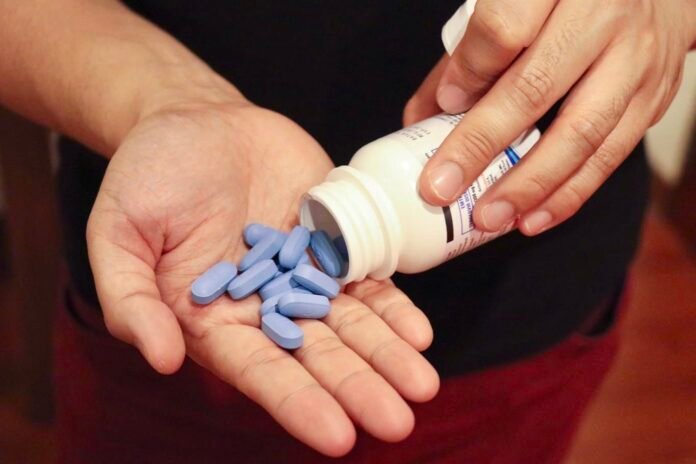
Forty-year-old Thulisile Nkosi* carefully counts the pills in her bottle before handing over a few to her friend.
”The tablets in the bottle are 28, so when I give her, I make sure I have some left until my next appointment.”
The pills are PrEP — pre-exposure prophylaxis — the daily medication that prevents HIV infection when taken correctly. Nkosi often shares them with her friend.
“I don’t ask a lot of questions, I just give her pills as she asks,” she says. “We drink alcohol together, sharing is caring, I am being neighbourly, I do not want to make her feel insecure.”
“It is normal here in our community to share PrEP treatment, because we are protecting each other.”
PrEP stokvels
Across Soweto, Finetown and Orange Farm, people who use PrEP have formed informal “stokvels”, where members pool resources to help each other.
Stokvels are usually money-saving clubs. But in these southern Johannesburg communities, PrEP users are quietly trading pills amongst themselves – sharing with friends who’ve missed clinic appointments, collecting on behalf of others and reselling.
“This system is a backup plan for patients who have missed their appointments to collect their monthly supply, and are scared to go and start the procedure from scratch,” explains one user from Finetown who asked not to be named.
“They may be afraid because they have already engaged in risky sexual behaviours, or nurses will scold them for missing their appointment and embarrass them in front of other patients.”
The risk in sharing pills is skipping doses, which undermines the protection PrEP offers.
Risky business
Mamello Mokoena, a prevention and treatment literacy promoter at the Treatment Action Campaign, warns that PrEP only works when taken as prescribed, and users must avoid skipping their daily dose.
“PrEP needs to be taken at least seven days before engaging in unprotected sex for the medication to work,” she explains.
Ex-eThekwini clinic employee accused of selling government-issued ARVs
“Even after those seven days, one doesn’t stop taking PrEP. An individual on PrEP must get their prescription refilled, and get a medical check-up, including HIV-testing, in the first three months of taking the treatment.”
The system keeps people away
Health-e News spoke to people who take PrEP, who mentioned several barriers to accessing the drug consistently, and avoiding the clinic.
Some mentioned clinic appointments clashing with work schedules.
“The slow-moving queue is boring because collecting PrEP should not be a long process,” one user says. Another said her partner refuses to let her take PrEP due to stigma.
In Soweto, 21-year-old Tshepiso Sithole* says she was given PrEP at the clinic after receiving a negative HIV test.
“I wasn’t there for PrEP but family planning, so after experiencing side effects from family planning, I was scared to take PrEP and gave it to my friend,” she says.
“This is a common trend among my friends. We collect PrEP for each other or even pay each other to go get some.”
Sithole says she worked at a college from 2024 to 2025, where a mobile clinic would provide PrEP and family planning services to students weekly.
“My male friends who were studying at the college would collect pills for our female friends, because the staff at the mobile required the young women to be on family planning to get PrEP,” she says.
South Africa’s PrEP guidelines state that anyone who identifies themselves at risk of HIV infection may request PrEP, and do not list family planning as a requirement.
“This trend did not stop when I left the college. Even now, some of my male friends still go to the clinic to collect PrEP to resell or to give to their girlfriends.”
Sithole says she would also go and collect PrEP if one of my friends has an emergency and needs a supply, or sell it to whoever needs it.
Mixed messages from health bodies
The South African National AIDS Council says it’s not aware of people exchanging PrEP medication. “Even civil society organisations have not reported the behaviour to the council,” says SANAC’s Nelson Dlamini.
“However, as the council, we will be engaging with the Department of Health, as they are the managers and implementers of the medication.”
Dlamini stressed that PrEP use needs to be monitored closely and that it’s illegal to sell the medication as it is available for free at government health facilities.
Chairperson of the Civil Society Forum of the Johannesburg AIDS Council, Tshepo Lekwape tells Health-e News it has anecdotal reports of people “sharing or pooling PrEP medication, particularly where access barriers exist. We do not have verified prevalence data, as this is not a formally tracked practice.”
Both Dlamini and Lekwape say they will engage with the health department and other partners to raise awareness about this practice, as well as work with the community to highlight the risks of sharing HIV prevention drugs.
“Inconsistent use or use by someone with undiagnosed HIV can contribute to drug resistance,” warns Lekwape. “Medicines distributed outside the formal supply chain may be expired, counterfeit, or stored incorrectly.” – Health-e News