By Tian Johnson, African Alliance, and Fatima Hassan, Health Justice Initiative
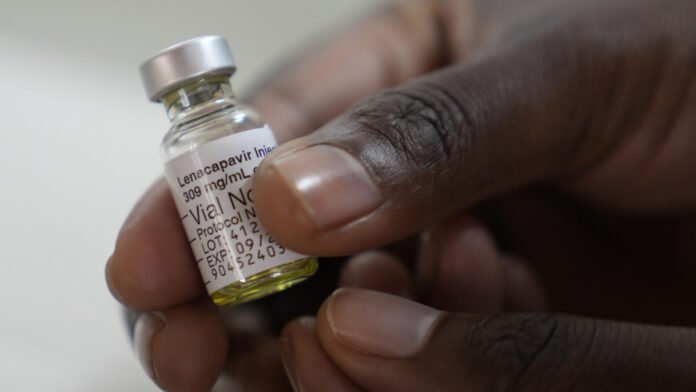
South Africa is being asked to celebrate a breakthrough that hasn’t happened yet. A plan to deliver lenacapavir (a groundbreaking HIV prevention injection) to roughly 400,000 people in our country has been framed as a turning point in the country’s HIV response. But all of the donated doses are not yet in hand, the rollout has not begun at scale, and the gap between promise and delivery remains wide.
We are managing HIV with selective lenacapavir roll-out, not ending it
The government’s recent call under the auspices of the South African National AIDS Council (SANAC) for expressions of interest to manufacture lenacapavir locally is being framed as a decisive step forward. In reality, it is the beginning of a long and uncertain process that uncritically hands immense power to the monopoly holder of lenacapavir: Gilead Sciences.
According to the Expression of Interest, published on 5 March 2026, local manufacturing companies are invited to apply (again). SANAC will shortlist and assess the proposals and then pursue license negotiations with Gilead. Only if those negotiations succeed with Gilead directly will a license be granted on terms that are not yet defined and not controlled by South Africa. Only then can production begin. Only after that will regulatory approval be sought. Contrary to what UNITAID has suggested, this, in reality, is not likely to take place within a year (the other 6 licensees are not yet on the market, those licenses were issued a while back, and not a single one is on the market yet, including the Egyptian one).
The HIV epidemic will not respect this timeline. South Africa continues to record hundreds of new HIV infections every day. Yet the response being constructed moves at the pace of committees, approvals, negotiations, and conditional agreements. There is no binding timeline for when locally produced doses will reach those who need them the most.
- No commitment on how many doses will be produced each year.
- No clarity on what they will cost.
- No clarity on whether patients outside of state facilities can access them too, and how.
- No clarity on whether South Africa will be permitted to supply countries outside of Africa that Gilead excluded from previous licensing arrangements.
In an active epidemic, these shortfalls will have real consequences.
Worryingly, the Expression of Interest is notably silent on whether SANAC’s shortlisting decisions are binding. If, as has been suggested by insiders, final approval rests with Gilead Sciences, enabling them to veto any shortlisting by SANAC, then the process risks reducing national actors to facilitators rather than decision-makers.
A manufacturing plan without control
The SANAC Expression of Interest process makes one thing clear: the outcome of this initiative does not sit in South Africa’s hands, despite all of the promises of multi-stakeholder review and engagement, and premature celebratory news headlines. The looming shadow of Gilead, whose track record prioritises profits over access, is very much staring us in the face.
Local manufacturing does not equal independence. In this case, it will depend on whether a seventh voluntary licence is indeed granted, on what terms, and on access to knowledge and inputs that remain controlled elsewhere. At no point in the process is there an enforceable guarantee that local production will actually proceed, let alone at the required scale.
This arrangement also risks reducing SANAC to an administrative clearing house. It convenes, consults, and coordinates, but it does not make decisions. The license, if granted, will be issued under terms set by Gilead Sciences, which will maintain control over pricing, volumes, and the pace of scale-up. Consequently, the South African government is left implementing a programme whose most critical parameters are decided elsewhere. That is not a partnership.
South Africa may host the factories and assemble the product. It may carry the burden of delivery. But without authority over all aspects of licensing, including pricing and scale, it does not control the outcome.
This creates a peculiar kind of progress in which South Africa prepares to build capacity without knowing whether it will be allowed to use it fully. It invests in a future supply chain that it does not yet govern. It signals ambition while accepting uncertainty at every critical point.
This dynamic has defined the relationship between African countries and global health innovation for decades. The work happens here: the trials, the data, the mobilisation of communities, the building of delivery systems. When a breakthrough emerges, the continent is (maybe, eventually) invited to participate in its production, but rarely to determine its terms. We saw this during the COVID-19 pandemic with drug companies in their local licensing arrangements, even dictating the end destination for locally manufactured supplies. Lenacapavir is beginning to follow that same script.
Capacity without guarantees
The local licensing announcement and proposal focus on capability: infrastructure, compliance, and technical readiness. It asks who can produce. It does not answer who will be protected. There are no binding commitments yet on production volumes. No indication of how many people will actually receive it each year. No targets linked to the number required to interrupt transmission. There is also no defined price, no ceiling, no mechanism to ensure that locally produced doses will be affordable at scale or assurances that, apart from South Africa and the region, other countries left out by Gilead that need access will benefit from South African manufacturing too.
Without these elements, manufacturing does not automatically translate into equity or access. It can just as easily reproduce scarcity under a different label.
The question is not whether a licence will be signed, but what that licence actually guarantees and delivers. The South African government could have taken compulsory measures, but so far, it has chosen not to. So now the programme details will be up to Gilead’s lawyers, not in the hands of the Health Minister, SANAC, or even the President.
This is nothing new. Too often, voluntary license arrangements presented as breakthroughs fail to translate into access. They lack enforceable timelines, guaranteed volumes, real price commitments, and meaningful technology transfer. They provide false hope.
A licence that shifts production without shifting power changes very little. The test is simple: does it reduce infections in the next two years, or does it defer them?
The question South Africa has not answered
There is a way to read the current moment as pragmatic. Manufacturing takes time, systems must be built and standards must be met. All of this is true. But pragmatism has a way of hardening into acceptance. And acceptance, in a country with South Africa’s burden of disease, worsened by the U.S. government’s punitive HIV funding cuts, carries a concrete cost.
South Africa is doing the work required to make a life-saving technology available. But whether that work will result in access at the scale and speed required to interrupt HIV transmission is not something it can yet guarantee. That is the contradiction at the heart of this effort. A country at the centre of the HIV epidemic is building a system it does not fully control, on a timeline it does not set, for an outcome it cannot yet secure.
This is not how epidemics are ended.
______________________________________________________________
Tian Johnson is the founder and strategist of the Pan-African health justice advocacy group, African Alliance. Fatima Hassan, is a South African human rights lawyer and social justice activist, and founder of the Health Justice Initiative. This is part 2 of a two-part opinion series by Johnson and Hassan examining the gap between scientific breakthrough and public health impact in South Africa’s response to HIV with the arrival of long-acting lenacapavir.
The views and opinions expressed in this opinion piece are those of the author, who is not employed by Health-e News. Health-e News is committed to presenting diverse perspectives to enrich public discourse on health-related issues.